Tennis is among the socially distanced sports that have been deemed low-risk for COVID-19 transmission. As such, popularity is growing, with an increase of 44% new participants during the pandemic. There is no denying the numerous benefits to your overall physical and mental health from playing tennis!
.
Unfortunately, injuries to the shoulder, elbow, ankle, and thigh are common, and adult players are at increased risk for low back pain and knee injuries.
.
H&D was pleased to host a discussion with Alexis Chiang Colvin, MD, Chief Medical Officer of the U.S. Tennis Association, and H&D’s own Aaron Huppert, PT, Cert MDT, about steps you can take to reduce your injury risk and what to do if an injury does occur.
.
The interactive hour-long discussion covered:
Tennis injury risk factors
Tennis-specific strength and conditioning program for injury prevention
Common tennis injuries and how we treat them
.
Thursday, March 25th
5pm – 6pm
.
Alexis Chiang Colvin, MD
.
Aaron Huppert, PT, Cert MD
Traumatic skiing and snowboarding injuries can affect multiple body parts including your spine, knee, ankle, shoulder, pelvis, wrist, and hands. Overuse injuries are also widely reported including shin splints, back pain, patellofemoral pain, Achilles tendonitis, and ankle and wrist sprains.
In 2019, knee injuries are the most reported injury in skiers, ranging from 27 to 41 percent of all injuries.1 Of this, ACL and MCL injuries make up 10% to 33% of all ski related injuries. A review by the American Academy of Orthopaedic Surgeons (AAOS) found that 92% of snowboarding injuries were caused by falls.2 Other causes of injury from Alpine sports can include fatigue, muscular imbalances (leg dominance), improperly fitting equipment, and collisions.
Upper extremity injuries are more common among snowboarders while lower extremity injuries occur more often among skiers. This is explained by the differing equipment used and mechanisms of falling. Forward falls from snowboards result in dislocations of the shoulder whereas skiers are more likely to injure their knees and thumbs.
Preparing the body to be as efficient as possible begins before you go. The ideal program should be targeted to muscular endurance, overall strength, and enhanced balance. Performing these activities year-round will allow your body to properly respond to the unusual demands of these snow sports.
A sport-specific conditioning program covers major muscle groups and mimic motions on the slopes to assist in preventing these common winter sports injuries and keep you feeling your best on the slopes.
As with all exercise programs, you need to use common sense when performing your routine and start every session with a proper warm up. It is always advisable to check with your doctor before beginning any fitness program.
Better. Begins. Here. Let us help you stay on the slopes longer and prevent the risk of injury from skiing and snowboarding with sport-specific conditioning. Try this simple Y balance test to assess your readiness for the slopes:
- Place tape on the floor in the shape of a Y or place three markers on the floor.
- Stand on one leg with your knee slightly bent and move the other leg in each direction along the Y (forward, side, behind) as far as you can.
Y Balance Pre-Test:
If you are having difficulty controlling any portion of the movement, please contact H&D Physical Therapy to schedule a screen. We will work with you to design a personalized sport-specific program that addresses your specific needs.
References:
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6299353/
- https://www.researchgate.net/publication/321580362_Comprehensive_Review_of_Skiing_and_Snowboarding_Injuries
For more tips, join us for a free webinar on January 20, 2020 5PM:
“Hit the Slopes Safely and Stay Injury-free this Winter“
Dizziness, imbalance, and falls are a significant problem for older adults and one of the most common reasons for hospitalization or visit to the doctor. An estimated 95% of hip fractures are due to falls and an older adult dies every 15 minutes due to injuries from a fall—this is a 30% increase over the past decade.
Are you feeling a bit overwhelmed by the thought of falling? Change your mindset from being on the defense and only treating imbalance and falls after they occur to being on the offense with these 5 simple actions.
- Talk openly with your primary health care provider
Falling or losing your balance can be stigmatizing. You may feel uncomfortable displaying vulnerability or you fear worrying loved ones. Don’t blame yourself; it is impossible to prevent all falls. More than 1 in 4 older adults fall each year but less than half tell their doctor. Falling once doubles your chances of falling again and increases the possibility of serious injury.
If you’ve had a fall or experienced dizziness, at your next appointment have the following discussion with your health care provider:
- Offer details about your falls and balance history. There may be medical factors influencing your balance systems that could be addressed. Early detection leads to early intervention and prevention of falls.
- Review all prescription and over-the-counter medications as certain medications are linked to an increase risk for falls. Older adults who take 4 or more medications are more likely to fall.
- Ask about taking vitamin supplements to improve bone, muscle and nerve health. Vitamin D and magnesium deficiency can increase your fall risk.
- Get your eyes examined
See an ophthalmologist immediately if you experience changes in your vision such as clouded, blurred or dim vision or sensitivity to light and glare. Your eyes are extremely important for balance and stability. Conditions such as cataracts, glaucoma, or macular degeneration, can increase your risk for falling. According to research, obtaining early cataract surgery, in just one eye, can significantly reduce your chances of falling.
Schedule an appointment for an annual eye examination to check for changes in your vision. If you need glasses, get them. If you wear glasses or contacts, check to see if your prescription should be updated. If your glasses are scratched or broken, replace them.
- ‘Fall-proof’ your home
Many falls occur in the perceived safety of our own homes. Hard and wet floors make the kitchen and bathrooms the most dangerous rooms in the home. Take the time to ‘fall-proof’ every room in your house. Determine which areas can be made safer with the following adjustments:
- Reduce clutter and remove anything you can trip over from stairs and walkways
- Remove or safely secure throw rugs with double-sided tape; use non-slip mats in the bathtub and shower
- Improve the lighting in your home, especially in poor-lit areas; use light-weight curtains, shades or blinds to reduce glare from windows
- Move items you use frequently in easy reach to minimize use of a step stool
- Install grab bars and handrails in high-risk areas (bathroom, stairs).
- Exercise daily
Exercise is proven to be extremely beneficial with reducing the risk for falls. Although exercise can provide tremendous benefits with respect to improving balance and fall risk, not all exercises are beneficial. A multi-component exercise program that addresses balance, strength, flexibility, and endurance is most effective. Click here for a step-by-step guide to 6 balance and strengthening exercises to get you started.
We also offer a weekly online group balance and exercise class. Learn more and make a reservation HERE.
Tai chi exercise has also demonstrated strong fall prevention results. Tai chi is an ancient Chinese martial art which is practiced globally for its various health benefits. It involves meditative and purposeful movements which often require people to move and shift their bodies into repetitive and very functional positions. You can find tai chi instructions and videos online or take classes, sometimes offered for free in community-based settings.
- Schedule a physical therapy evaluation
Our body systems have a pesky way of weakening and slowing down as we get older. Taking that ounce of prevention now can slow or even reverse some of these processes. If you have fallen or are concerned about falling, consultation with a physical therapist is recommended.
A physical therapist can perform a comprehensive evaluation of your balance and musculoskeletal systems and provide you with personalized assessment of your risk for falls and individualized exercises aimed at improving your stability.
We do not have to accept falling as an inevitable part of aging. Implementing any of these 5 strategies has been proven effective in reducing the risk of falling. We hope you start with at least one today.
For more information, click HERE to access the video recording of the webinar Prevent Falls with Better Balance
By Dr. Kathy Uy, PT, DPT, CFMT, OCS
As the COVID-19 pandemic rages on, so does our neck and back pain. Proper office ergonomics — including correct chair height, adequate equipment spacing and good desk posture — can make working from home more comfortable. Here are some tips to make your home work space work for you.
Start by creating a designated work space and then make modifications to support good posture.
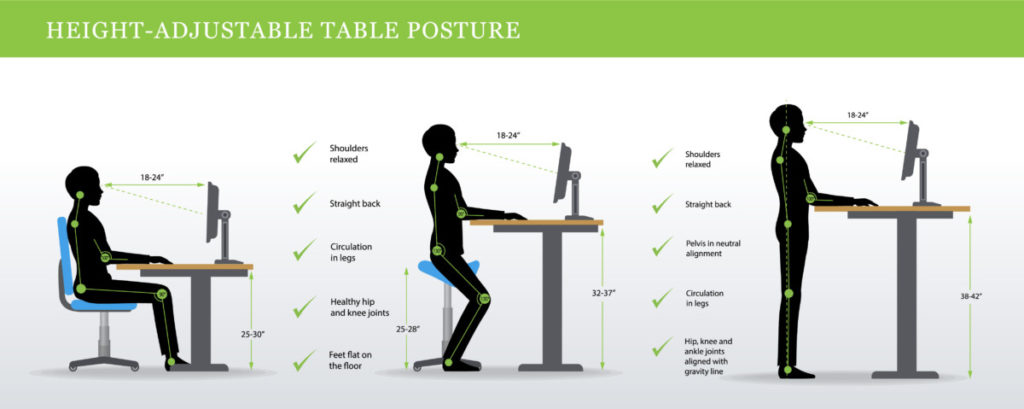
Seating: Whether you are working at a desk or kitchen table, sitting in a chair with a straight back helps you avoid slumping and provides needed support to your back and neck. Adjust the chair height so your knees are about level with your hips.
Make sure you can sit back in your chair with your feet resting on the floor. If the chair is too deep, you can place a pillow or firm cushion behind you. If the chair is too high, place a book or footstool under your feet.
Proper arm support decreases pressure on your neck and the load on your back. If your chair has arm rests, keep your elbows close to your body with a 90 to 120 degree bend. If you use an armless chair, tuck a pillow into your lap to support your elbows
As you work, check periodically to ensure you’re sitting back in your chair with shoulders dropped , rolled back and relaxed.
Computer monitor: Check the height and distance of your monitor. Placing the monitor an arm’s length away with the top of the screen at eye level prevents craning, squinting, slouching along with decreasing eye and muscle strain. Sturdy books , a ream of paper, a monitor riser or adjustable laptop stand all are good options to help you hit the ideal height. Try tilting the screen to find the optimal angle for easy reading. Consider a desk lamp to reduce glare.
Keyboard and mouse: When using the keyboard and mouse, keep your wrists straight and your hands at or below elbow level. If you are using a laptop, once the monitor is at eye level, the keyboard will be too high and an external keyboard is necessary to prevent wrist pain. The external keyboard should be placed within easy reach on the desk as close to you as possible.
Cell phones: The stress in your neck muscles caused by repeatedly tilting your head to hold your phone can cause neck pain or spasm. Prop your phone up in front of you on a stand or against something sturdy and use the speaker function, if possible. If privacy is needed, earbuds with a microphone or a wireless bluetooth headset leave you hand’s free to multitask while maintaining good posture.
Finally, structure breaks from your work area and move around. A recent study reported that 37% of remote workers stayed productive by taking short breaks during their work day. Keep your muscles loose and joints less stiff by standing up or walking about every 30-45 minutes. Give your eyes a rest by looking away from your computer and focusing on a distant object multiple times throughout the day.
When you cannot leave your desk, take a few deep breaths and perform simple stretches. Your eyes and body will thank you.
If you have any questions or would like to connect to make an appointment, please click on the button below!
Join us for a free webinar on Oct 21, 2020 5PM:
“Working from Home during the pandemic; Expert Tips and Treatments to stay pain-free“
During the first 6 months of the COVID-19 pandemic, New York City saw over a 60% increase in bicycle ridership. Bike shops were deemed an essential service as the city shut down. However, as riders biked more miles than ever before, there was an increase in cycling-related repetitive strain injuries.
Preventing pain starts before your ride. Dr. Labelson has created this simple warm-up program for cyclists targeting the hamstrings, hips, quadriceps and spine.
As with all exercise programs, you need to use common sense when performing your warm-up. It is always advisable to check with your doctor before beginning any fitness program.

See the full slide presentation by clicking on the button below:
View the recorded replay by clicking this button below:

By Dr. Shara Labelson, DPT, CEAS
2020 has certainly had its challenges. My year began with a death in the family, leading to a diagnosis of “acute thyroiditis.” Just as I was getting my energy back, NYC got devastated by COVID-19 and a global pandemic. With New York shut down, and my move to all telehealth, I found more time to spend on my trusty friend, my bicycle. Why not make the best of an otherwise unfortunate circumstance?
Typically, in March, my bike racing season starts. That means, from January on, a program of very structured training including 4am wake ups to get on the bike for leg and lung busting workouts before work. I had no idea how I was going to be in shape to race after my thyroiditis, but as all racing got canceled, and cycling stayed an essential activity, I began to increase my miles and focus on my overall health and not just race shape.
The first thing I wanted to focus on was proper sleep. During sleep is when our body recovers and repairs to be ready for the next day. It is important for cognition, concentration, problem solving, reaction time, and overall performance (mentally and physically). On the flip side, poor sleep has been found to be correlated with an increased risk of type 2 diabetes, heart disease, depression and stroke.
The next item on my list was diet. With time to regularly go grocery shopping and cook proper meals at home, I wanted to make sure that I was eating a proper balance of fruits, vegetables, whole grains, healthy fats and lean protein. I had to make sure my body had the proper fuel for my daily rides. You cannot run your car on an empty gas tank. (It seems you also can’t take away my nightly ice cream fix though)
As a physical therapist, I always try to practice what I preach. I educate patients on the importance of stretching and strengthening in order to prevent injury. The most common injuries from cycling are tendinitis of the hamstring, quadriceps, and Achilles tendons and neck and low back pains. Some of these issues can be resolved with a proper bike fit. A saddle being even a few millimeters too high, low, forward, back, can lead to pain after miles of pedaling.
If the bike is not the issue, we must look at imbalances within ourselves. I began to pull out my yoga mat in the living room daily to foam roll and stretch my quads, hamstrings, calves and especially my tight hip rotators. With an increase in sitting during COVID, keeping the pliability of these muscles has become even more paramount. I also concentrated on trying to even out the strength imbalance between my right and left legs. Exercises for this included single leg bridging, clamshells and reverse clamshells, Bulgarian split squats and single leg calf raises.
To stave off back and neck pain from the increased miles being bent over on my bike and sitting in front of the computer, I challenged my friends to a plank challenge and added on other posture exercises including wall angels, shoulder external rotation with bands, and prone scapular stabilizations exercises.
Heading into fall, I was feeling like I was in the best shape of my life! I took a trip to the Catskills (not quite the Dolomites that I was planning for this summer to celebrate my birthday) to conquer a few mountain passes with some riding comrades who prefer the hills WAY more than I do. As a racer that usually competes in flat, sprint type races, this was quite the accomplishment. I did not have my companions waiting too long for me even at the top of the last over 4-mile climb with an elevation of 1,624 feet and gradients over 20% as we neared the summit.
Now you ask, the title of this is “Advice from an injured bike racer,” so what happened? And after all of this if she is injured why should we listen to her? There is one BIG variable that you cannot account for in cycling. What happens when you do not, as we say, stay rubber side down? Two weeks ago today, I was out riding and enjoying the sun on my face and wind through my helmet vents, when, as I crossed an intersection an 18 year old driver decided that he was going to make a right turn, cutting me off and knocking me off of my bike. Of all the possible outcomes in this scenario, I am happy to be writing this with left arm in a sling after only suffering a separated acromioclavicular joint and slightly sprained wrist.
So I guess the moral of the story is stay as healthy as you can to prevent injury, but sometimes stuff happens and when it does, being otherwise in good shape, will help you return to sport as fast as possible. I will end up with a bump on my shoulder that will slow me down for a few weeks, but I’ll be back!
~By Michelle Troiano, PT, DPT
Physical Therapy through Zoom may not seem like it would be helpful to figure out how to fix those aches and pains, but it has proven to be as effective as going to a clinic. Multiple studies have analyzed the benefits of teletherapy for patients with musculoskeletal pain, including post-op, chronic back pain, and arthritis, and found real-time telerehabilitation to be comparable to standard practice with high satisfaction rates.
When you schedule an initial evaluation with a licensed therapist, you can expect a thorough examination starting with a history of your problem areas and visual examination. This can include assessing for range of motion, strength, balance, and form with functional movements. After identifying your individual needs and determining a proper diagnosis, you will be taken through a series of self-treatment techniques and prescriptive exercises tailored specifically for you with the guidance of your therapist at every step of the way. Through video, the therapist can modify your movement patterns, answer questions, and provide proper instruction without even having to leave the house. No equipment necessary, just the creativity of using household items to assist in your rehabilitation.
Want to see the research, no problem, click HERE, HERE, and HERE!
If you are interested in scheduling an appointment for telehealth, please click on the button below.
~ H&D Physical Therapy presents ~
Alternatives to Surgery;
Regenerative Medicine in 2020
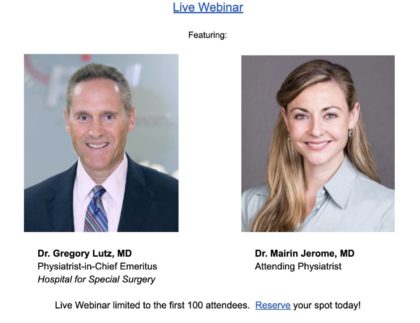
Elective surgeries have re-emerged under the current COVID-19 landscape. However, many patients are turning towards non-operative procedures to alleviate their pain. New research in the field of regenerative medicine using prolotherapy, platelet rich plasma (PRP), and stem-cell injections has revealed very promising outcomes. Join Dr. Gregory Lutz, MD and Dr. Mairin Jerome, MD, of Regenerative SportsCare Institute (RSI) as they explore the growing field of Regenerative Orthopedic Medicine. Topics will include an overview of the approach to patient care at RSI, as well as treatments for specific cases related to the spine, hip and pelvic pain.
Tuesday, August 4th
5pm – 6pm
Live Webinar
Featuring:

Dr. Gregory Lutz, MD
Physiatrist-in-Chief Emeritus
Hospital for Special Surgery

Dr. Mairin Jerome, MD
Attending Physiatrist
Live Webinar limited to the first 100 attendees. Reserve your spot today!
We are pleased to share our updated library on YouTube, filled with patient experiences, testimonials, walkthroughs, helpful health tips, wellness advice, workouts, and fitness tips. Today, we’re sharing this playlist featuring all of our exercise oriented videos.
Please remember, if you’re attempting to try any of these as an address to your health — the right pairing of motion to syndrome should cause fairly quick resolution. If you’re not getting the anticipated results, you just might need one of our provider’s to take a look and hear out your story on how you got here in the first place.
Enjoy!
First & foremost, we would like to extend our most sincere wishes to you, your families and loved ones that you are safe and healthy, and are making it through this crisis without too much hardship. Fortunately, the staff at H & D Physical & Occupational Therapy are healthy at this time. Since the onset of “shelter in place”, we have been offering significantly reduced office hours supplemented by Home Visits and our New TeleHealth and TeleWellness services. Given that NY State Department of Health considers PT’s and OT’s to be an essential service and more of us are ready to return to work, we will be gradually expanding our office hours and reopening all of our offices. This will be for patients who require our services in person and are comfortable coming to and returning to the offices.
We are reopening our Midtown office and expanding staffing and hours at our 88th St and Yorkville offices on Monday May 18, 2020. We would like to make you aware of the following precautionary procedures that have been instituted to ensure everyone’s safety. Given the ever changing nature of this situation, certain aspects of these protocols may change over time.
In accordance with New York State Department of Health laws, everyone who enters the office will be required to wear a face mask. Our entire staff will also be donning face masks.
We will provide hand sanitizer to everyone who enters the office, and will require each individual to thoroughly wash and/or sanitize hands upon entry.
We will take the temperature of every individual entering the office utilizing a no-touch infrared thermometer. If an individual is found to have a temperature above 99.6 F, s/he will be asked to reschedule their appointment for another time and be instructed to contact their primary care physician (PCP).
We will observe recommendations for physical distancing by spacing out appointments to avoid having more than 1 or 2 patients in the waiting area at any time (depending on which office you go to). Following initial screening, you will be escorted to a private room or the gym depending on individualized treatment and/or therapist.
We will observe all recommendations for infection control regarding the cleaning procedures of all surfaces that patients and therapists come in contact with.
We request that you attend your visits alone. We recognize that there may be situations when this is not possible. If that is the case, we request that you inform us at the time you are scheduling your appointment. We will address each circumstance on an individual basis. The assessment will be done by our clinical policy and procedure team which has been set up in advance to address these type of issues.
In summary, our COVID-19 safety protocols are as follows:
- Prioritizing Cleanliness: All rooms and high touch areas will be disinfected frequently. Disinfectants, hand sanitizer, and related supplies will be available to staff and patients at all times. Staff will open doors for all patients, and wash hands between each patient interaction.
- No ‘waiting rooms’: Patients will be asked to arrive when it is time for their appointment to avoid waiting.
- Staggered Appointments: We will be staggering the appointments to ensure adequate time to wipe down spaces in order to maintain a safe and clean environment.
- Screenings: We will be screening patients over the phone and at the time of their appointment to ensure they are healthy.
- Reduced & Healthy Staff: Any of our staff who can work virtually will be working outside of the office, and all staff will be screened daily to ensure they are healthy.
- Protective Equipment: Our staff and patients with appointments will wear a mask and gloves at all times. We ask that all patients come to their appointment with a mask!
If you have any questions concerning the information contained in this correspondence, please feel free to contact us at anytime. Thank you for your cooperation in these matters. We really have missed and look forward to seeing you when you feel safe in returning!
Sincerely,
Entire Staff of H & D Physical & Occupational Therapy








You must be logged in to post a comment.